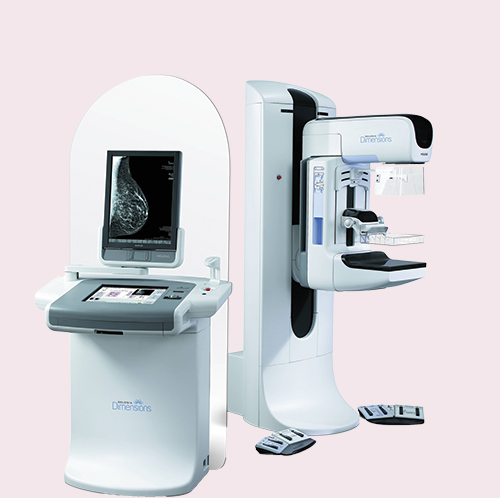
3D Mammogram
Mammography is currently evolving at a rapid pace. Mammogram screening guidelines are continually being refined, and 3-D technology is replacing standard 2-D digital mammograms.
Convenience, service, and quality are becoming increasingly important factors in the delivery of effective healthcare and reimbursement models.
MammoLink® continually analyzes and anticipates breast cancer screening trends and proactively ensures our physicians are aligned with a successful practice now and in the future.
Guidelines
Breast cancer screening with mammography remains one of the great success stories of modern medicine. Science has repeatedly proven that early detection of breast cancer saves lives. Without question, 3D mammogram is not going anywhere soon. Despite this, many patients and physicians are being inundated with confusing and seemingly conflicting headlines regarding mammogram breast cancer screening guidelines.
Despite variation in mammogram age and screening interval recommendations from some groups, including the United States Preventative Services Task Force (USPSTF), overall there remain more similarities than differences from most healthcare organizations. For example, The American Medical Association (AMA), the Society of Breast Imaging (SBI), the American College of Radiology (ACR), the American Congress of Obstetricians and Gynecologists (ACOG), the American Cancer Society (ACS), and the National Comprehensive Cancer Network (NCCN) all continue to support annual screening with mammography, most beginning at age 40. In any event, the practice patterns in the United States continue to favor these traditional mammogram recommendations and the patterns do not seem likely to change anytime soon.
All major insurance carriers continue to reimburse for annual mammogram screening beginning at a clinically appropriate age. MammoLink® supports annual routine screening alongside these mammogram recommendations, but defers to the expertise of our physician partners in their respective clinical settings.
Technology
Breast tomosynthesis/3D mammogram continues to play an increasingly important role in breast cancer screening and appears poised to eventually replace standard 2-D digital mammography as the standard of care. This is similar to how 2-D full field digital mammography replaced analog film screen in the first decade of this century.
Numerous scientific studies have now demonstrated the benefits of 3D mammogram. Among them, a study published in the Journal of the American Medical Association (JAMA) in 2012 involving nearly half a million women demonstrated a significant increase in the breast cancer detection rate and the simultaneous decrease in the recall rate with breast tomosynthesis when compared to standard 2-D digital mammography. In January of 2015, Medicare was the first insurer to begin reimbursing for breast exams. More recently, in August of 2016, Cigna, inspired by the mammogram recommendations of the National Comprehensive Cancer Network (NCCN), became the first private insurer to begin reimbursing for breast tomosynthsis. More recently, as of April 2017, Anthem and UnitedHealthcare have also reported that they will reimburse for 3D mammogram. Largely as a result of recent studies documenting cost saving and increased breast cancer detection rates, several states including New York, Texas, New Jersey, New Hampshire, and Maryland have introduced bills seeking mandated insurance reimbursement for patients seeking to undergo breast tomosynthesis in their states. In the future, as the technology becomes more widespread, there will likely be an increasingly larger network of insurance companies that reimburse for breast tomosynthesis. 3-D digital mammography units (all of which are capable of standard 2-D digital mammography) ensure that our physician partners remain capable of providing the best services to their patients now and in the future.
Quality
The healthcare delivery system in the United States is becoming increasingly criticized for the “gap” between what we know to be good healthcare and the healthcare that people actually receive. This “gap” was first defined and addressed by the National Academy of Sciences, Institute of Medicine, in 2001 with the publication of their landmark report, Crossing the Quality Chasm: A New Health System for the 21st Century. The report outlined six aims to help bridge the gap to a better healthcare system. According to the report, quality healthcare should be safe, effective, timely, efficient, patient-centered, and equitable.
MammoLink® is proud to redefine traditional mammography by providing a better “link” between patients, physicians, and breast exams imaging radiologists in the field of breast cancer mammogram screening. Currently, MammoLink® is in the process of working with the academic breast imaging community to quantitatively better define the benefits of this relationship with its own groundbreaking study in an attempt to become recognized as the “gold standard” for quality breast cancer screening in the United States. As both private and government insurance reimbursement models become more selective based on quality, MammoLink® is thereby ensuring that our physician partners will be successful and recognized as leaders in quality diagnostic mammogram healthcare now and in the future.

- -Free financial feasibility analysis
- -Physical site design and logistics coordination
- -IT and EHR planning and integration
- -Equipment installation
- -State and Insurance registration
- -ACR certification
- -New program marketing
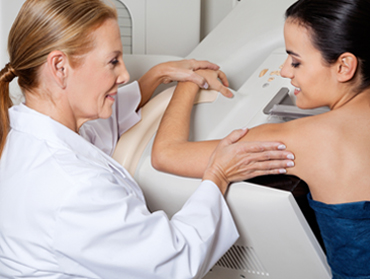
- -State of the art 3D breast tomosynthesis mammography unit capable of standard full field 2D digital imaging
- -Screening and Diagnostic mammography capability
- -Mammography Technologist work station
- -Cloud based high speed PACS
- -Long term mammography compliant storage solution
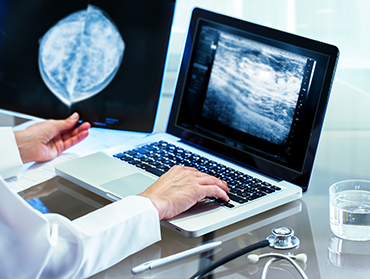
- -Board certified fellowship trained and dedicated breast imaging radiologists from major academic institutions
- -If preferred outside radiologists can be considered if meeting MammoLink® standards
- -Fully insured licensed and credentialed, Malpractice and liability coverage paid by MammoLink®

- -Mammography technologists certified by the American Registry of Radiologic Technologists (ARRT)
- -All mammography technologists employed and managed by MammoLink®
- -Mammography technologists selectively recruited with expertise in ACR and MQSA/FDA standards and regulatory compliance

- -MammoLink® ensures complete regulatory compliance with all legal and accrediting bodies
- -MammoLink® coordinates and oversees all mandatory American College of Radiology (ACR) and Food and Drug Administration (FDA) inspections
- -Instantaneous mammographic interpretation and reporting

- -MammoLink® provides complete equipment and IT support
- -Legal expertise made available to our physician partners
- -Regularly scheduled conferences according to the preference of the physician group
- -Quarterly satisfaction reviews provided

